As sustainability becomes more and more understood as a smart business practice, medical device companies that proactively incorporate sustainability in their product development process, will be ahead of the game.
In the first article in this series, we looked at the overall landscape of sustainability in the medical device world. We developed an understanding of how we define “sustainability” and how regulatory, societal, and corporate pressures are encouraging medical device companies to become proactive and incorporate sustainable thinking into their product development practices. While patient safety will always be the primary requirement in the medical world, there are opportunities for creating solutions that are great for patients and practitioners, and that benefit the planet and the bottom line in the process.
After the last article’s look at materials, this article shifts the focus to packaging. As with other aspects of medical device design, medical packaging has its own unique set of challenges.
- Sterility.With patient safety at the top of the list of product requirements, ensuring sterility is a must for a wide array of medical devices. These challenges include selecting materials that can withstand sterilization and ensuring that seals remain impenetrable to infectious agents.
- Usability.Sterile medical devices must be easy to handle and open with gloved hands. The packing has to make it simple to transfer the device into the sterile field. It’s also important to guard against loose parts tumbling off the instrument table and coiled items unfurling awkwardly and out of control.
- Distribution.While all products have distribution challenges, medical products have to work within the supply chain and storage practices of hospitals and other medical facilities.
Sterilization
As an essential element of ensuring patient safety, sterilization deserves a more in-depth discussion. There are three main kinds of sterilization used with medical devices: autoclaving with steam, irradiation, and Ethylene Oxide (ETO) sterilization. Autoclaving is primarily used with metal devices, like surgical instruments, intended for extensive re-sterilization and reuse. Irradiation and toxic gas sterilization are used with plastic disposable devices that can’t withstand the heat in an autoclave.
There are two kinds of irradiation sterilization—gamma ray and electron beam. Gamma rays leave no residues behind and, since the rays penetrate deeply, packaging materials don’t need to be permeable. Gamma irradiation works well even for products with high density. Electron beam radiation doesn’t penetrate deeply, so it’s best used with low-density products that are packaged with uniform thickness and densities. If using irradiation, it’s important to select plastics like polycarbonate which doesn’t break down as easily when exposed to these energy rays.
ETO sterilization requires the device to have a permeable membrane that lets the ETO gas flow into the package and through the device itself in order to kill any microorganisms that may be present. The gas is then evacuated from the packaging. Devices packed in trays sealed with a Tyvek top layer have typically been sterilized with ETO, as Tyvek, provides the “just right” permeability that let’s ETO in and out of the package, and keeps microorganisms out.
 Preserving safety, improving usability, and increasing sustainability
Preserving safety, improving usability, and increasing sustainability
Even more than consumer products, medical products are often nested within several “layers.” The “primary packaging” in medical devices is designed to preserve sterility and often includes a “belt and suspenders” approach with a sterile package enclosed inside another sterile package. This article includes a story of the redesign of Medtronic’s stylet kits. The original kits had a Tyvek-topped tray, packed within a second Tyvek topped tray, and then packed inside a carton. After the redesign, the packaging was reduced to a pouch packed inside a DVD cover. This reduced the materials required for the two inner elements and entirely eliminated the need for the carton.
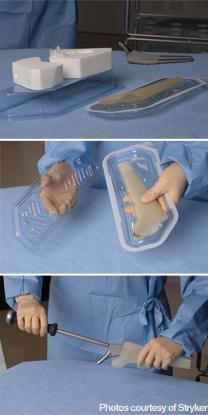
The redesign of the packaging for the Stryker hip stem is a wonderful illustration of how integrating packaging design into the development of the whole user experience can preserve safety, reduce waste, and even improve the medical procedure itself. Previously, the stem had been cradled in thick foam pieces in a plastic blister tray which was sealed with Tyvek. The redesign completely eliminated the bulky foam pieces. Instead the stem was packaged in open-ended polyurethane pouch. The hip stems are encased in abrasive coatings so they can be installed without cement. The pouch system not only resulted in a package less than half as thick as the original, it became part of the procedure, allowing the surgeon to safely grip the stem at a critical point in the procedure.
Is it time to fire the Gorilla?
 Before closing, I’d like to zoom out to the big picture view for a paradigm-shifting idea. It’s an idea that pushes beyond just medical packaging to all kinds of packaging and the shipping industry as a whole. What if we do away with the gorilla-tested model of packaging? Remember the old American Tourister commercial with luggage tough enough to stand up to being tossed about and stomped on by a gorilla? Packaging standards have long been based on a similar premise: make sure the shipping package can withstand abuse in transit—whether that’s being crammed into a cargo container, tossed across a warehouse, or knocked about in the back of a delivery truck.
Before closing, I’d like to zoom out to the big picture view for a paradigm-shifting idea. It’s an idea that pushes beyond just medical packaging to all kinds of packaging and the shipping industry as a whole. What if we do away with the gorilla-tested model of packaging? Remember the old American Tourister commercial with luggage tough enough to stand up to being tossed about and stomped on by a gorilla? Packaging standards have long been based on a similar premise: make sure the shipping package can withstand abuse in transit—whether that’s being crammed into a cargo container, tossed across a warehouse, or knocked about in the back of a delivery truck.
It’s a system built on a decades old paradigm. Today’s shippers are highly-automated, and this automation can result in a kinder, gentler ride for any package. In theory, if packages received “padded glove” treatment, they wouldn’t need to be so padded themselves, and a great deal of excess packaging could be eliminated.
Impossible? Maybe. But I believe we’re long overdue for a re-evaluation of our current shipping paradigm. Taking a big step back and reconsidering our assumptions can help us make the kind of impact necessary to ensure our future.
Additional references:
- MedTech Innovation: Building Sustainability into Medical Packaging by Nicholas Berendt
- American Tourister Commerical info.







