With the advent of COVID-19, all aspects of life have changed, including healthcare education. Due to the pandemic, there has been an increased reliance on robot-like patient simulators for training.
Healthcare education encompasses a broad spectrum from undergraduate student clinical training to in-service training for experienced medical professionals. COVID-19 forced a reimagining of all of these segments of training. For students, the impact on education concerns the required clinical time in hospitals. Normally students gain some of their practical experience through hands-on training at clinical sites. The pandemic has prevented access to these sites. Clinical simulation provides a vital alternative for training. Students practice both clinical skills and critical thinking on lifelike patient simulators that reproduce a patient’s clinical condition. This allows the learner to gain valuable experience with new techniques long before they advance to a true clinical situation.
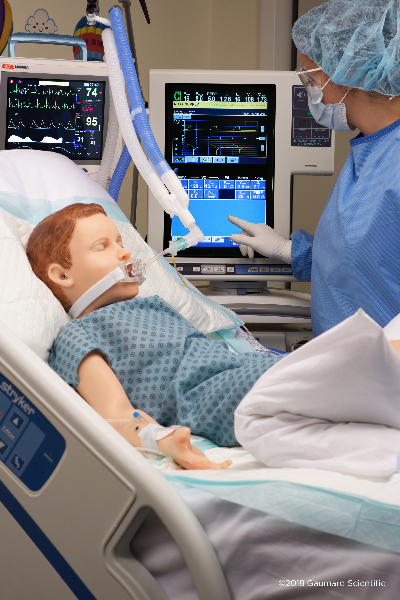
The need for simulator training for in-service education of existing healthcare professionals is growing at a rapid pace, and has been amplified by COVID-19. Hospitals are experiencing a surge of COVID-19 patients, and nurses are being cross-trained in new areas in which they may have no prior work experience or training. For example, a nurse who previously worked in the post-surgical unit, routinely caring for patients post-op, is now thrust into an intensive care unit to treat patients with COVID-19 complications. That nurse may not have proper training in maintaining a patient that is ventilated. In this scenario, training with a patient simulator provides valuable experience by exactly reproducing the complications of a ventilated patient in a critical care setting.
Simulation Training for COVID-19 Patient Care
A study published by the National Council of State Boards of Nursing’s (NCSBN) found that training with simulation is as effective as clinical training with a patient in training nursing students.1 In fact, NCSBN authorized up to 50% of the students’ clinical time could be done via simulator in an optimally designed simulation training program. The utility of simulation has also been proven in many other disciplines, such as airline pilots who train on flight simulators long before they enter an airplane cockpit, and surgeons that train on surgical simulators before they ever conduct surgery.
Sophisticated scenario-based patient simulators allow for advanced critical thinking training by replicating the clinical experience. The goal is for the learner to be completely immersed in a scenario so that he or she believes they are treating an actual patient. This is achieved by producing a simulator that looks and feels as realistic as possible through capabilities such as eyes that move and blink, pupils that constrict and dilate, voice activation and a head that moves and turns. In addition, these high-fidelity simulators have pulses, breathe, have heart rhythms and blood pressure that can be detected and displayed on real medical equipment, just as on live patients. These features engage the emotions of the learner and provide a very realistic learning environment, allowing the learners to be immersed in the exercise and treat the simulated patient just as they would a live patient. Practice and repetition in these high stress environments with patient simulators trains the learner to make critical split-second decisions.
For COVID-19 training, many of the clinical requirements have been in cross-training professionals in respiratory care, intensive care and critical care. Medical professionals learn how ventilators and respirators work by training on a simulator that responds to ventilation. In order for mechanical ventilation to be effective, a patient must have an open airway for an endotracheal tube to be inserted directly into the trachea. Thus, for a simulator to accurately reproduce this patient, it must have an open airway and a chest that rises and falls. These critically ill patients often exhibit chronic illnesses such as COPD, bronchitis or emphysema. Likewise, the simulator must be able to reproduce these chronic illnesses to accurately represent inhalation and exhalation.
Since this critically ill patient is sedated, additional skills are required for proper care. These include maintaining the endotracheal tube described earlier or inserting a gastric tube for feeding. Many nurses who have been reassigned to critical care from other areas may be unfamiliar with these skills or need to be refreshed. Clinical simulation provides the optimal training adjunct so skills can be practiced on a patient simulator before that nurse is required to care for a patient.
The Future of Patient Simulators
Patient simulators have been used for training since the 1950’s and have continued to advance since then, from a basic skills trainer (still in use) to a full body interactive robot. In the current COVID-19 healthcare environment, education is changing rapidly due to an increase in distance learning. The technology of some simulators today allows learners to train in clinical skills remotely. A simulator can be controlled by an onsite instructor and an entire class of students can be trained on a scenario and provide feedback remotely. For example, a birthing simulator could be operated by one person onsite but many learners can be remotely observing the birth. If there is a complication, it can be addressed, resolved and repeated to ensure comprehension of the learners.
More advanced simulators allow learners to use mixed reality viewer lenses to visualize the internal anatomy of a simulated patient. With these lenses, students can learn skills not just through observation, but through remote active participation.
Advanced technology has allowed sophisticated simulators to:
- Operate for hours on a single battery charge
- Be controlled wirelessly by a tablet that is more than a football field away
- Provide vital signs to real patient monitoring equipment
- Reproduce critically ill patient conditions and respond to therapeutic intervention
- Allow learners to view the internal anatomy of a patient and integrate this into their learning model
- And now incorporate distance learning strategies into clinical training
The industry has been moving in that direction, and COVID-19 has put it on a fast track and forced the methods of clinical education to be restructured to ensure optimal competency of the next generation of healthcare providers.
References
- Hayden, JK. (2014). The NCSBN National Simulation Study: A Longitudinal, Randomized, Controlled Study Replacing Clinical Hours with Simulation in Prelicensure Nursing Education. Journal of Nursing Regulation. 5(2), S3-S40.







